The evolution of sperm donation and egg freezing, from early artificial insemination to cutting-edge fertility solutions. As reproductive technology advances and societal values shift, these techniques are reshaping the future of parenthood. But what’s driving this growing demand?



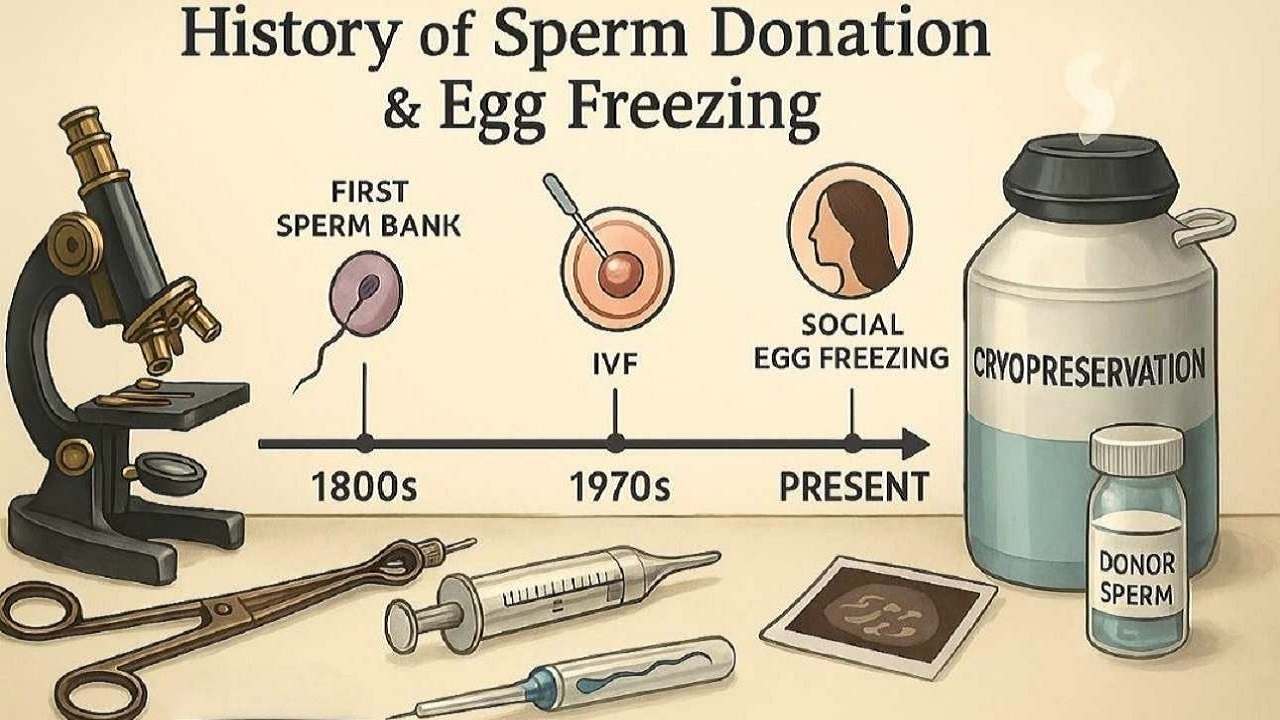
Advancements in reproductive medicine have profoundly changed the way we view family planning, fertility, and family creation. Two key advancements in this area sperm donation and egg freezing gave individuals and couples the ability to combat infertility struggles, postpone having children or seek other family-building solutions. Both have been critical to assisted reproductive technologies (ART), helping people conceive when they otherwise could not. Sperm donation and egg freezing are two of the most commonly used techniques in fertility care; this article traces the history of sperm donation and freezing techniques, exploring how they emerged, evolved and became common elements of fertility care all over the world.
The practice of sperm donation in its modern form can be traced back to the late 19th and early 20th centuries. The notion of artificial insemination (AI), the process of inserting sperm into a woman’s reproductive tract without sex, entered the scientific zeitgeist during this period. In the late 1800s, Dr. William Pancoast and a few others started conducting experiments around artificial insemination methods, but the results of early attempts were predominantly animal-based.
The first human artificial insemination dates back to the early 20th century when some fertility pioneers began working on ways to address the condition of male infertility. Early approaches were often crude and lacking in insight into the preservation of or selection for sperm. Now, even if male infertility was the underlying problem in the couple, sperm from a female partner was often used in the early procedures.
The idea of breeding with someone else’s sperm was popularised during the 1950s with the introduction of anonymous sperm donation, leading to artificial insemination. Sperm banks made it a more systematic process. In America, it all started in 1947 with the opening of the New York Cryobank, the first formal sperm donation clinic. That opened the door to storing and using sperm from healthy, anonymous donors to assist women and couples who were experiencing male infertility or wanted to embark on childbearing without a male partner.
Sperm donation was still controversial at this point, as the use of donor sperm at the time raised ethical concerns about the anonymity of donors and the implications of creating children without a biological connection to the intended parent. Nonetheless, the supply of men willing to provide sperm donations expanded, as demand rose from women and couples considering ART solutions for their dreams of parenthood.
Sperm banks became increasingly sophisticated by the 1970s, including standards for screening donor health and genetic background. This was significant as it helped alleviate concerns regarding the quality and safety of donor-derived sperm. Moreover, the application of semen analysis and sperm washing techniques, which were developed for the assessment and purification of sperm, optimised artificial insemination success rates and enhanced the safety of sperm donation practices.
The birth of Louise Brown, the first baby conceived in a laboratory dish using in vitro fertilization (IVF), in 1978 opened a new world for fertility treatments. With IVF, sperm from donors could be used alongside egg retrieval from women. This trend normalised sperm donation as a viable option for building a family for single women, lesbian couples and heterosexual couples dealing with male infertility.
The late 20th and early 21st centuries saw sperm donations used as part of a wide range of fertility treatments. Egg and sperm banks proliferated, and sperm donation was integrated into the fabric of fertility care. From there, the ethical debates over issues such as whether to allow anonymity, the right of children to know their biological origins, and how to regulate sperm bank conspiracies gained steam.
In recent years, there has been a movement for open-identity sperm donation, whereby children born from donor sperm can access identifying information about their donor once they reach a certain age. This shift indicates an increased social understanding of the significance of genetic identity and of the rights of donor-conceived people.
Sperm donation is now a common practice, millions of children have been born using donor sperm, and sperm banks are well regulated across the world. Sperm donation has become a common service provided by ART clinics, assisting people having difficulties with male infertility, single women wanting children, and same-sex couples with family formation.
Egg freezing, or oocyte cryopreservation, also became a beacon for women who want to preserve their fertility. But the concept of freezing eggs for later use didn’t come along until the 1970s and 1980s. The first successful experiments in human egg freezing was performed in the late 1960s and early 1970s, but the procedure, at first experimental and often unsuccessful, was not widely available. The issue was that, in contrast to sperm, eggs are much larger and more complex, so freezing them without harming their internal structures was a struggle. But the real breakthrough came in the 1980s when those scientists started experimenting with ways to freeze and thaw human eggs without wrecking the cells. This is when the slowly freezing technique started to develop; this method immersed the eggs in lower temperatures over time.
Over the course of the 1990s, egg-freezing techniques improved, with scientific refinements of cryopreservation methods and a better awareness of how to maintain the integrity of the egg through the process of freezing it. But egg freezing didn’t start gaining traction until the late 1990s and early 2000s, when it became adopted in the mainstream fertility industry. The technology was still in development, and egg freezing was mainly an option for women who were about to undergo medical treatments, such as chemotherapy, that could threaten their fertility.
Even though the technology had improved, rates of success for frozen egg retrieval and fertilization were still fairly low, and it wasn’t until the introduction of vitrification (a rapid freezing method) in the 2000's that the procedure truly became much more effective. Vitrification, in which the amniotic fluid is replaced by a viscous solution, prevents the formation of ice crystals inside the eggs, one of the big reasons freezing eggs had posed such a challenge. Vitrification also increased thawed egg survival, resulting in improved fertilization and pregnancy rates.
The most notable milestone in the history of egg freezing arrived in the 2010s, as improvements in freezing methods, alongside societal recognition and evolving cultural values surrounding the female biological clock, rendered egg freezing an increasingly popular option for non-medical purposes (which is often categorized into the group "social egg freezing"). Egg freezing began to be seen by many women as a means of preserving their fertility while they pursued careers, education or the right partner.
In 2012, the American Society for Reproductive Medicine (ASRM) removed its experimental label from egg freezing, acknowledging the procedure as an established form of fertility preservation. It was a momentous occasion in the annals of egg freezing, one that cemented the technique’s role within the field of mainstream fertility medicine.
By the 2020s, egg freezing had developed into a widespread practice, with fertility clinics marketing it to women who wished to postpone childbearing without sacrificing their chances of having a child later in life. Some companies, particularly in the tech industry, have started to offer egg freezing as a benefit for employees to assist women in extending their reproductive options.
In the realm of reproductive medicine, sperm donation and egg freezing have emerged as essential tools, providing individuals and couples with greater autonomy over their reproductive health and options for family-building. The rising demand for sperm donation and egg freezing will continue to impact the future of ART, particularly as increasing advancements in genetic screening, cryopreservation technology, and societal changes related to childbearing and family building emerge.
Considering the ethical debates surrounding donor anonymity, genetic screening, and accessibility, difficult conversations that may shape the future of sperm donation and egg freezing, these discussions will continue, driven by innovation, medical advancements, and a commitment to making fertility treatments more accessible to an increasingly diverse population.
Sperm donation and egg freezing have a long history that reflects the progress of reproductive medicine and awareness of fertility. From the first experiments with artificial insemination and cryopreservation to the practice of egg freezing for social reasons, these techniques have changed how people approach family-building. As reproductive technologies continue to evolve, the future looks even brighter for those who wish to do everything from preserve their fertility to use new and innovative methods to create their families.
