The differences between Mini IVF and traditional IVF, focusing on success rates, medication dosages, and cost-effectiveness. Learn how minimal stimulation protocols prioritize egg quality to offer a less invasive path to parenthood for specific patient profiles.



In the sophisticated landscape of Assisted Reproductive Technology (ART), the journey toward parenthood has evolved from a singular path into a nuanced selection of medical strategies. For professionals and executives navigating this complex terrain, the decision often hinges on balancing medical efficacy, physical impact, and resource allocation. At the center of this dialogue is a critical comparison: the refined, low-intensity approach known as Mini IVF versus the robust, high-yield methodology of traditional In Vitro Fertilization (IVF).
As fertility care becomes increasingly personalized, understanding these distinctions is not merely a matter of medical curiosity but a strategic necessity. While traditional IVF remains the global powerhouse for successful outcomes per cycle, the emergence of minimal stimulation protocols offers a compelling alternative for specific patient profiles, prioritizing "quality over quantity."
Mini IVF, or minimal stimulation IVF, represents a paradigm shift in reproductive medicine. Rather than overriding the body’s natural cycle with aggressive hormone regimens, this approach seeks to work in harmony with the patient’s biological rhythm.
The core of the Mini IVF protocol lies in its pharmaceutical strategy. Unlike traditional methods that rely heavily on daily gonadotropin injections, this milder version utilizes:
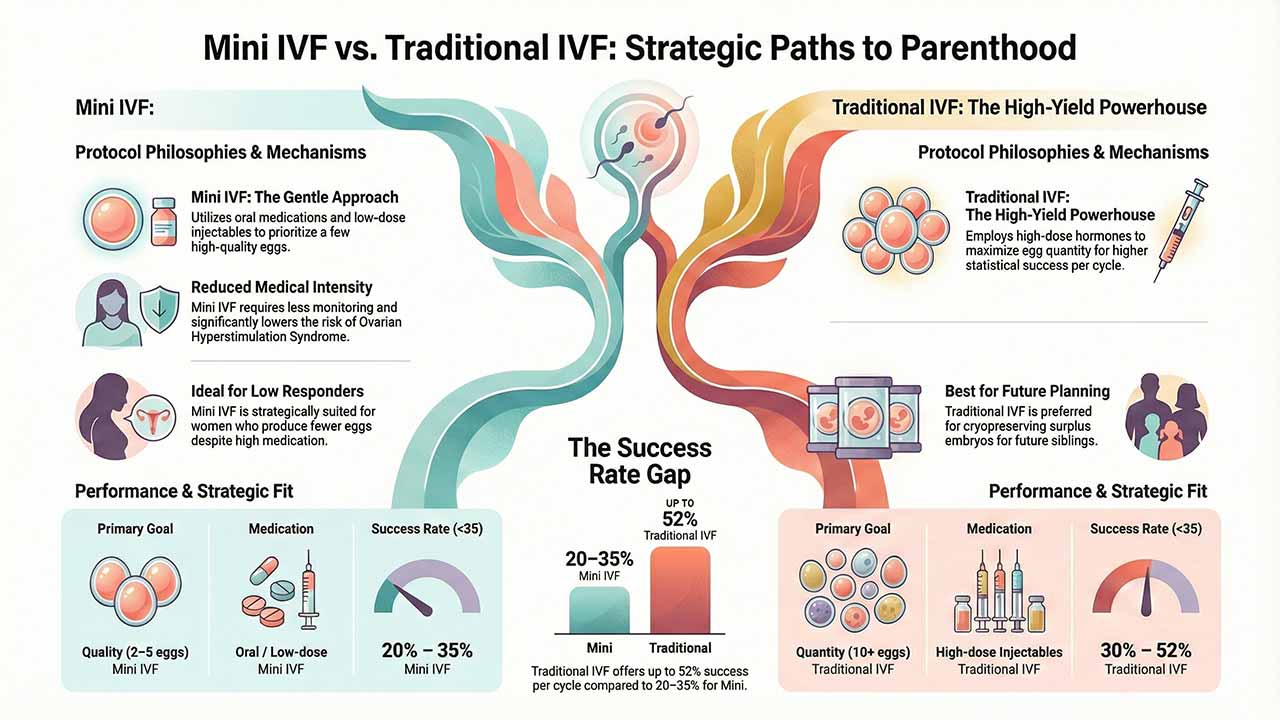
The objective of Mini IVF is not to produce a large volume of eggs, but rather to retrieve a select few (typically 2 to 5) that represent the highest potential for viability. By avoiding high-dose hormones, the procedure significantly reduces the risk of Ovarian Hyperstimulation Syndrome (OHSS), a condition characterized by painful swelling of the ovaries that can occur when stimulation is too aggressive. For many, this "gentle" approach is less invasive and reduces the physical and emotional strain often associated with fertility treatments.
While the minimal approach offers finesse, traditional IVF remains the established "gold standard" for those seeking the highest probability of success in a single clinical attempt.
The strategic goal of traditional IVF is the retrieval of a significant number of eggs, usually 10 or more, in a single cycle. This is achieved through a high-dose protocol of injectable hormones (FSH and LH) that stimulate the ovaries to produce multiple follicles.
This methodology, while highly effective, demands a greater commitment. The costs are naturally higher due to the significant volume of medication required and the intensive monitoring needed to track follicle development and safeguard the patient's health. Furthermore, the physical demand, multiple daily injections and frequent clinic visits, can be more taxing for the patient.
When evaluating Mini IVF against traditional IVF, the primary metric of interest for most is the success rate. However, success must be viewed through both a "per-cycle" and a "cumulative" lens.
Statistics from the Society for Assisted Reproductive Technology (SART) and other clinical bodies indicate a clear advantage for traditional IVF in terms of immediate results. For women under 35, traditional IVF boasts a live birth rate of approximately 52%, whereas Mini IVF success rates typically hover between 20% and 35% per cycle.
However, the "cost-effectiveness" of the minimal approach can be deceptive. While a single cycle of Mini IVF is less expensive, the lower success rate per attempt means a patient might require three cycles to achieve what traditional IVF could accomplish in one. Over time, these multiple cycles can offset the initial financial and emotional savings.
Choosing the appropriate protocol is a highly individualized decision that should be made in close consultation with a fertility specialist. Factors such as age, ovarian reserve (determined via AMH testing), and specific fertility diagnoses (such as PCOS or male factor infertility) play a decisive role.
The transition from a "one-size-fits-all" approach to a nuanced menu of options marks a positive evolution in reproductive medicine. Mini IVF provides a sophisticated, gentler gateway for those who prioritize biological harmony and minimal intervention, while traditional IVF remains the robust engine of the industry, delivering high-probability outcomes for the widest range of patients.
Ultimately, the "right" choice is the one that aligns with your medical profile, your financial strategy, and your long-term family goals. By leveraging the data and the expertise of senior clinical consultants, you can navigate your fertility journey with the confidence and clarity that such a significant life decision deserves.
