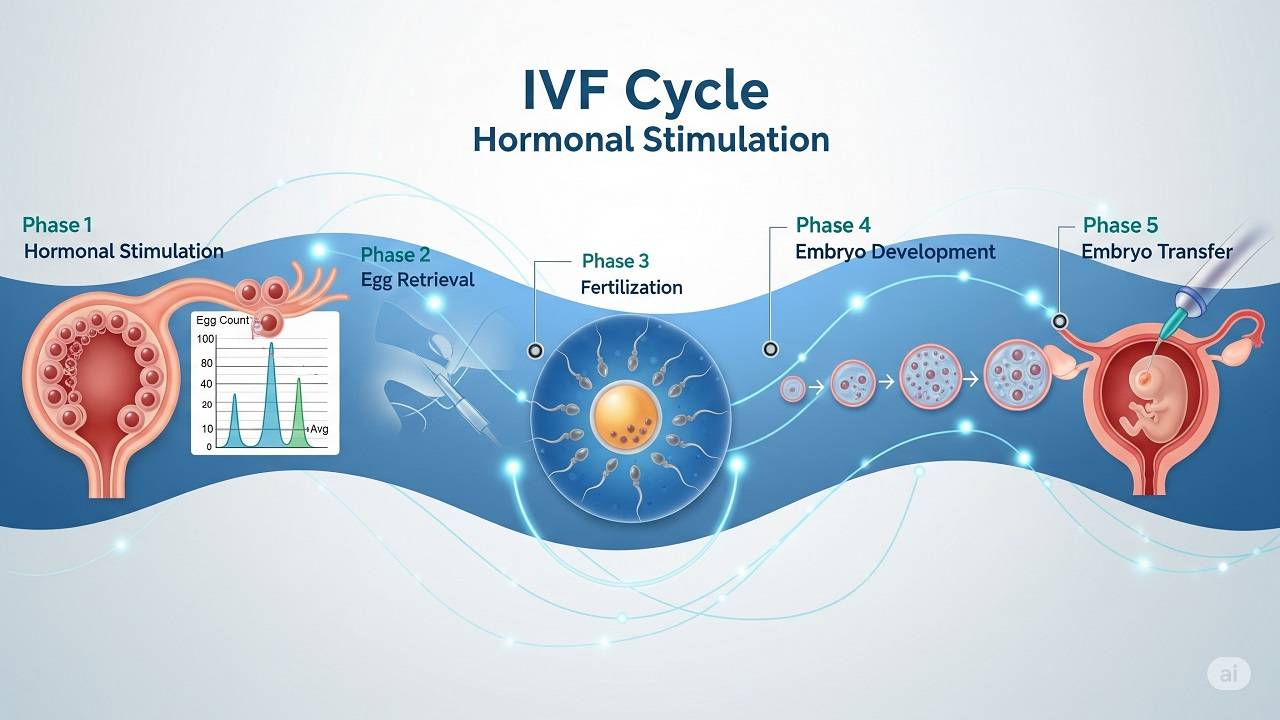
The In Vitro Fertilization (IVF) process emphasizes the importance of hormonal stimulation for successful outcomes. It explains how hormonal stimulation is crucial for ovarian development, enabling the production of multiple eggs for fertilization and ultimately enhancing the chances of achieving a successful pregnancy.
In vitro fertilization (IVF) is an effectively used ART (assisted reproductive technology), either as a standalone treatment or in conjunction with other techniques. There are several steps in the IVF process: ovarian stimulation, egg retrieval, fertilization, and embryo transfer. An IVF cycle relies heavily on hormonal stimulation to artificially induce the ovarian development of multiple eggs. As such, knowing about the IVF timeline and the process of hormonal stimulation can help individuals or couples undergoing IVF treatment feel more knowledgeable about what is to come.

IVF Cycle Timeline
Most IVF cycles take around 4 to 6 weeks from the start of ovarian stimulation (injections) to the pregnancy test. The time frame can differ somewhat depending on a handful of factors, including the age of the patient, how well they respond to medications, and the unique protocol the fertility clinic uses. Here’s a typical IVF timeline, divided into phases.
WEEK 1: Initial Consultation and Ovarian Suppression
- Pre-Treatment Consultation: The patient will do a battery of blood work, ultrasounds, and occasionally a hysteroscopy prior to embarking on the IVF cycle to evaluate fertility and overall reproductive health. These tests also provide information about the patient’s ovarian reserve (egg supply), hormone levels and uterine conditions.
- Ovulation Suppression: To regulate the ovaries before stimulation, the fertility specialist may prescribe oral contraceptives or a gonadotropin-releasing hormone agonist (GnRH agonist) for a short period of time prior to the start of stimulation. This is a step that helps synchronise ovaries and prevents over-early ovules during stimulation. The suppression phase usually occurs for 10–14 days.
Week 2-3: The Ovarian Stimulation
TThe ovarian stimulation phase is the most important part of the IVF cycle, as the patient starts a series of hormone injections to prompt her ovaries to develop multiple eggs at once.This stage usually lasts approximately 10 to 14 days.
- Ovarian Stimulation Initiation: After ovarian suppression, the patient begins gonadotropin injections (FSH – follicle-stimulating hormone, and sometimes LH – luteinizing hormone). These medications prompt the ovaries to produce several follicles, each with an egg.
- One of the most common tests performed is called monitoring. During ovarian stimulation, the patient usually has blood draws and ultrasounds in a reproductive Endocrinology office to monitor how the patient is responding to medication. Ultrasounds monitor the number and size of developing follicles, and blood tests measure levels of hormones, particularly estrogen. This enables the doctor to fine-tune medication dosages.
- If the ovaries are over-responding or under-responding to the medication, the fertility specialist may adjust the doses of gonadotropins. The goal is to stimulate the ovaries to produce multiple mature eggs without overstimulating them (a condition called ovarian hyperstimulation syndrome, or OHSS).
Week 3: Final Oocyte Maturation and Trigger Shot
Once the follicles have matured to the appropriate size (typically 18-20 mm in diameter), the final stage of ovarian stimulation commences.
- The doctor gives a trigger shot of human chorionic gonadotropin (hCG) or a GnRH agonist between Day 10 and 14 of ovarian stimulation to help the eggs mature. The trigger shot is important because it mimics the natural surge in LH that happens right before ovulation. The trigger shot must be timed so the eggs are ready to be collected.
- Timing of Egg Retrieval: Egg retrieval (also known as aspiration) happens around 36 hours after the trigger shot. That gives time for the eggs to mature and to be ready for fertilization.
Week 4: The Collection of Eggs and Their Fertilization
- Egg Retrieval: The Egg retrieval procedure is done under sedation or light anaesthesia. To retrieve the eggs, a needle is placed into the ovaries via the vaginal wall under ultrasound guidance. The process will take about 20-30 minutes. Recovery is quick, and the patient can return home the same day, however, the patient might feel mild cramping or spotting afterward.
- Fertilization: Once the eggs are collected, they are fertilized in the lab with either partner or donor sperm. This is often in conjunction with a technique called intracytoplasmic sperm injection (ICSI), which involves injecting directly into each egg a single sperm (if needed). The fertilized eggs (embryos) are then checked for growth and development during the following 3–5 days.
Week 4-5: Embryo Development and Transfer

Embryo Culture: Post fertilization, embryos are cultured in the lab for 3–5 days. The embryologist observes their development over the following days, looking for signs of healthy cell division and blastocyst formation (the stage at which the embryo is ready for implantation). The embryos are graded according to their appearance, and only the best-quality embryos are chosen for transfer.
Embryo Transfer: The last step is the embryo transfer, the non-surgical procedure in which the selected embryos are placed into the woman's uterus. The transfer is usually performed 3 to 5 days after egg retrieval, based on how well the embryos are developing. The embryos are carefully placed directly into the uterine cavity via a catheter, a relatively straightforward, painless procedure. Here, one or two embryos are transferred depending on the case of the patient (the number is often limited to prevent multiple pregnancies).
Weeks 5-6: Support the Luteal Phase and Pregnancy Test
Luteal Stage Sustenance: Subsequently, they start taking progesterone, which is generally administered through injections or vaginal suppositories, after the embryo transfer to help support the uterine lining and encourage embryo implantation. This stage generally continues until the pregnancy is confirmed with a blood test.
- Pregnancy Test: The patient performs a blood test (beta HCG test) to test for pregnancy approximately 10–14 days after embryo transfer. A positive test means that the embryo has implanted in the uterus, and the pregnancy is viable. The patient will get repeated blood tests and ultrasounds to confirm the pregnancy is viable and to monitor the early stages of pregnancy
The process of hormonal stimulation in IVF
Hormonal stimulation is necessary for IVF because it allows the ovaries to generate many eggs (and for these eggs to be fertilized), all the better to maximize the likelihood of success. Several key medications are involved in this process:
Gonadotropins (FSH and LH)
- FSH (Follicle-Stimulating Hormone): FSH promotes follicle production in the ovaries, and each follicle contains an egg. It is also the main hormone used to stimulate the ovaries.
- LH (Luteinizing Hormone): In certain protocols, LH is added to the mixture to support the egg maturation process. FSH has to do with early follicle development, but without it, the follicles cannot mature; LH works alongside FSH to ensure proper follicle development.
GnRH Agonists or Antagonists
- GnRH Agonists: These medications suppress the body’s natural hormone cycle to help stop premature ovulation. They are administered at the beginning of the IVF cycle to modulate ovulation prior to stimulation.
- GnRH Antagonists: These medications are administered later in the cycle to prevent premature ovulation during ovarian stimulation. Sometimes they are used in short IVF protocols.
Note: hCG (Human Chorionic Gonadotropin)
hCG is given to trigger the final maturation of the eggs just prior to retrieval. This hormone is similar to the body’s natural luteinizing hormone surge that happens in a typical cycle right before ovulation.
Progesterone
Progesterone provides luteal phase support following embryo transfer to maintain endometrial growth and succeed in the implantation of the embryo. Progesterone may be given through injections, vaginal suppositories, or oral medications.
Conclusion
In Vitro Fertilisation (IVF) is a complex multiple-step process with a series of good decision-making for a successful positive pregnancy. An important component of the cycle is the ovarian stimulation phase, in which hormonal medications are administered to stimulate the ovaries to produce multiple eggs. In addition, the process of hormonal stimulation takes care to ensure that an adequate number of eggs have matured in order to be available for fertilization, and monitoring the patient’s response to medication during treatment allows for optimisation of the result of the cycle. The timeline and role of hormonal stimulation may also be useful for patients in preparing for their IVF journey and may boost their chances of success.