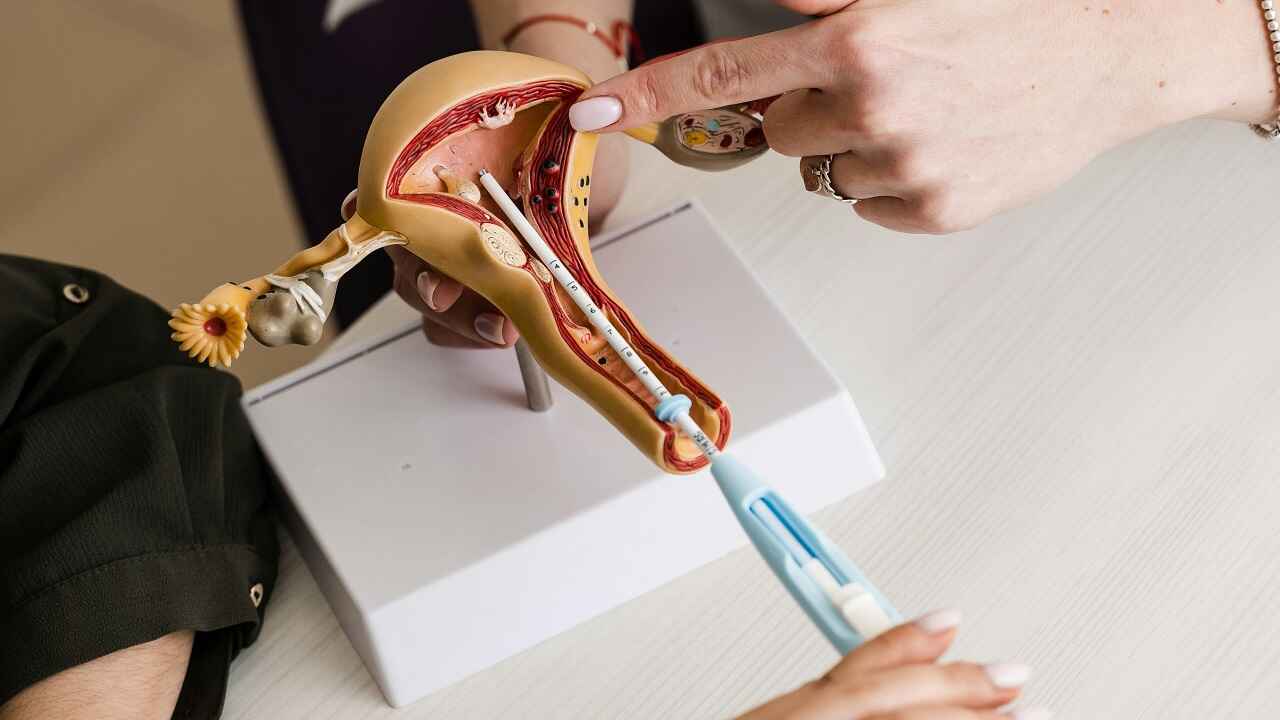
The Egg Retrieval Procedure details its importance in the In Vitro Fertilization (IVF) and Intracytoplasmic Sperm Injection (ICSI) processes for collecting mature eggs for fertilization. It outlines the steps involved in the Egg Retrieval Procedure, including ovarian stimulation, the actual retrieval method, and post-procedure care while addressing potential risks and complications.
Egg retrieval (also called egg aspiration) is a part of the assisted reproductive technologies (ART), IVF (In Vitro Fertilization) and ICSI (Intracytoplasmic Sperm Injection). This process consists of extracting mature eggs out of a female’s ovaries, which can be fertilized in the lab to generate embryos that could be transferred to the uterus. Women undergoing IVF or other fertility treatments need to understand the entire egg retrieval process, from preparation to recovery. We will break down the process:
What is Egg Retrieval?
Once the eggs have been stimulated to mature via hormone treatments, egg retrieval is the process by which those eggs get removed from a woman's ovaries. The objective is to collect as many eggs in a single cycle to maximise the odds of reaching fertilization and ultimately pregnancy. The procedure is usually done under sedation or anaesthesia to keep the woman comfortable.
The Steps Through Egg Retrieval

Ovarian Stimulation
The ovarian stimulation is performed prior to the egg retrieval procedure. That includes hormone injections that induce the ovaries to create several eggs. Typically, a woman’s body releases one egg in a cycle, but during IVF, the goal is to retrieve several mature eggs simultaneously to increase the chances for a successful outcome. During this phase, the hormones used are:
- Follicle-stimulating hormone (FSH): Stimulates the development of several follicles (the sacs in the ovaries that hold eggs).
Luteinizing hormone (LH): Matures the Eggs
- Human chorionic gonadotropin (HCG): Stimulates final maturation of eggs shortly before retrieval. Ovarian stimulation usually goes on for approximately 10-14 days. Over this time, the woman will be given multiple visits to the clinic for blood tests and ultrasound scans to assess the maturation of the ova and the ovarian stimulation response.
- Ultrasound and blood test monitoring: Follicular growth and development are closely monitored with transvaginal ultrasound and blood tests. An ultrasound provides the doctor with a way to measure the size of the follicles, and blood tests help gauge the levels of hormones, particularly estrogen, which increases as the follicles mature. When the follicles appear to be ready, the female receives an HCG injection to induce the final maturation of the oocytes.
- Timing of Egg Retrieval: Egg retrieval usually takes place 34-36 hours after the HCG injection. The timing is critical here, when the eggs are matured and ready to be harvested but not yet released from the follicles, since otherwise they'd be out of reach for fertilization.
Egg Retrieval Procedure (Aspiration)
The egg retrieval itself is a minor procedure, usually done at a fertility clinic. Here’s a step-by-step description of what happens in the procedure:
- Anaesthesia or Sedation: Egg retrieval is generally done under sedation or local anaesthesia. The patient is also often placed under light general anaesthesia so the procedure can be done with them comfortable and relaxed and often does not recall the procedure. The process can be accompanied by some pain, since they puncture the ovaries with a needle, and this helps reduce that discomfort during the procedure.”
- Transvaginal Ultrasound Guidance: To extract the eggs, the fertility specialist inserts a transvaginal ultrasound probe into the vagina to see the ovaries. The ultrasound shows real-time images of the ovaries and follicles. Using the ultrasound as a guide, a long, slender needle is inserted through the vaginal wall into the ovaries, and the eggs are aspirated (suctioned) from the follicles.
- Egg Aspiration: The needle is attached to a suction device, which gently removes the fluid in each follicle and the egg within. The eggs are then harvested in a test tube, and embryologists meticulously inspect the fluid under a microscope. Not all follicles will have an egg, and the number of eggs retrieved varies. A typical retrieval yields 8-15 eggs, but this number varies according to age, ovarian reserve, and ovarian stimulation response.
- Duration of the Procedure: The egg retrieval process itself normally lasts 20–30 mins. Although the process is quite short, it takes thorough monitoring during the procedure for the safety and comfort of the patient.
What Happens After the Egg Retrieval Procedure?
- Recovery from Sedation: The woman will be taken to a recovery room after the procedure, where she can rest while the sedation wears off. After the procedure, it’s normal to experience some cramping or mild discomfort; this is also true for bloating, which may persist due to ovarian stimulation. Most pain fades in a few hours. Most women are able to go home the same day, but it’s best to have a friend or family member with you, since you might still feel a little drowsy from the sedation.
- Post-Procedure Monitoring: For the next few days, the woman can have very mild spotting or light bleeding, and this is normal. The doctor may also check her hormone levels to make sure everything is proceeding normally. Most women are counselled to refrain from vigorous activities and intercourse during that time so that the body can gradually recuperate.
Embryo fertilization and development

Known as egg retrieval, the process is then immediately taken into the laboratory, where the eggs are then fertilized with the partner’s or donor sperm. With ICSI, though, the sperm is literally injected into the egg. The fertilized eggs (embryos) are then cultured for a few days to observe their development. The doctor decides the best timing for embryo transfer, usually 3-5 days after fertilization, depending on the quality of the embryos.
Risks and Potential Complications of Egg Retrieval
Egg retrieval is generally safe, but there are some risks involved, including
- Ovarian hyperstimulation syndrome (OHSS): In rare cases, stimulation of the ovaries can cause them to become swollen and painful. Severe OHSS can be life-threatening, but it is generally preventable with careful monitoring.
- Infection: There is a small risk of infection where the device is inserted, as with any surgical procedure.
- Bleeding: Minor bleeding is rare but can occasionally happen, especially if a blood vessel is unintentionally pierced with a needle during its insertion.
- Discomfort and Bloating: Some cramping, bloating, or spotting after the procedure is normal, and most women recover completely within a few days.
Conclusion
Egg retrieval (or aspiration) is a critical step in the IVF and ICSI process when doctors gather the mature eggs for fertilization and culture as embryos for transfer. It is minimally invasive, sedation is given, and the procedure is usually quick. Although it is not without risks, egg retrieval is a relatively safe and well-tolerated procedure, with most women recovering smoothly. But improvements in the science and technology of fertility medicine are helping to make it an easier process, with improved success rates for couples who want to start or expand their families.