Intrauterine Insemination (IUI) has played a vital role in advancements in fertility treatment, evolving from experimental use in the 1960s to a widely used clinical procedure. With innovations like sperm washing and ultrasound guidance, IUI continues to contribute to advancements in fertility treatment, offering a less invasive option for couples facing infertility.



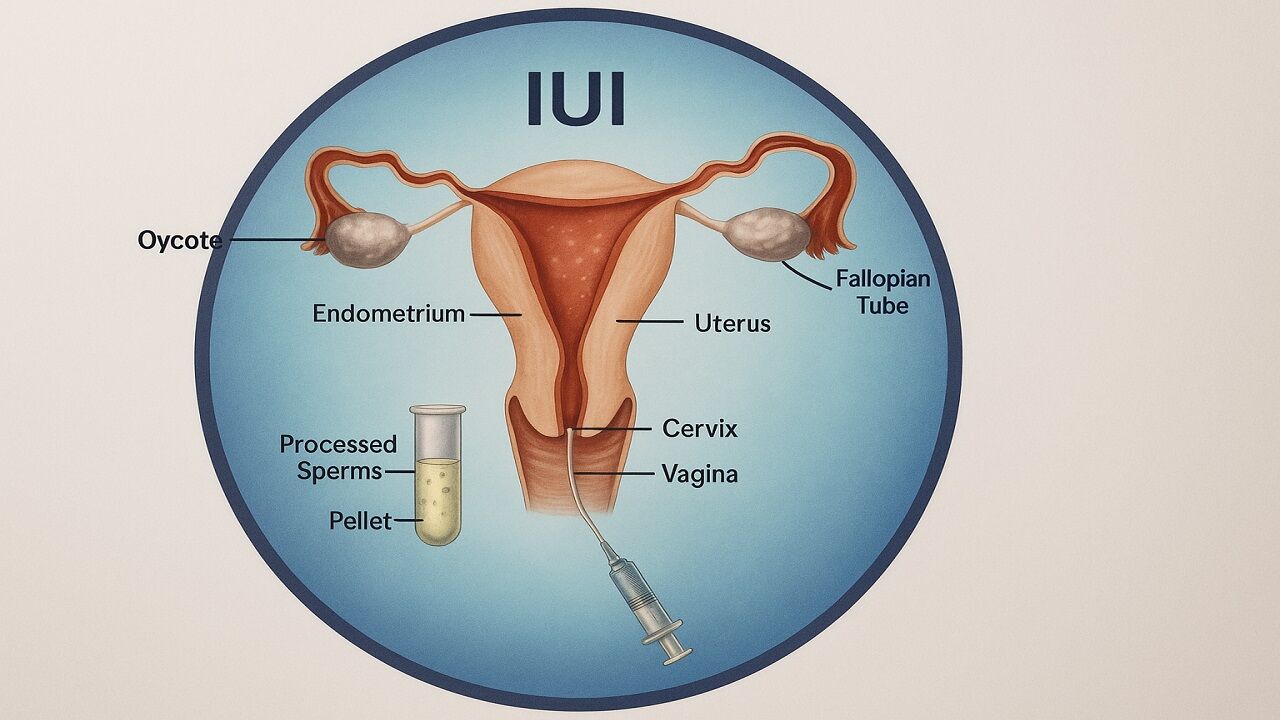
Intrauterine Insemination (IUI) is one of the most commonly used and available assisted reproductive technologies (ART) that couples face when they experience infertility. IUI involves inserting sperm into a woman's uterus, which gives the sperm a better chance of reaching the egg. It is now a routine procedure for treating specific types of male and female infertility. IUI has been developed and used clinically as a less invasive and more cost-effective alternative to other ART methods, including In vitro fertilization (IVF), demonstrating the advancements in fertility treatment over the decade. In this article I discuss when and how IUI was introduced for therapeutic use and how this treatment developed from early laboratory studies into a widely used fertility treatment.
Artificial insemination (AI) has its origins in ancient history. Records from as far back as the Greeks and Egyptians indicate that artificial insemination was at least contemplated in various ways, yet it wasn't until the 1900s that more advanced techniques were established. Modern artificial insemination techniques would not be possible without research into reproductive biology, sperm collection, and fertility treatment in the early 1900s.
The initial successes of artificial insemination occurred in animals, especially horses and cattle, where sperm could be directly deposited into the uterus. However, only during the mid-20th century were these kinds of techniques proven to work on humans, thanks in large part to the development of sperm preservation and medical processes that enable sperm to be harvested and stored in an effective manner.
Dr. Gregory Pincus, an American biologist, is generally credited with the clinical application of IUI in the 1950s. Dr. Pincus was their champion, and he went on to the birth control revolution: He helped develop the birth control pill that made his work not only possible but also practical. He was instrumental in establishing the concept that artificial insemination could be performed via intrauterine methods, as opposed to traditional methods for insemination, which involved placing the sperm in the vagina.
Before IUI, techniques for artificial insemination generally involved placing sperm in the cervix or the vagina and leaving it to swim up to the egg on its own. But this approach wasn’t very practical, particularly in cases of sperm motility problems or other fertility issues. This is where IUI came into play, and it increased the chances of sperm and egg meeting by inserting sperm directly in the uterus closer to the fallopian tubes, where fertilization occurs. This direct placement and increase in sperm concentration allowed for greater potential to fertilize.
Though IUI as a concept was developed in the 1950s, it was not until the 1970s that the procedure started being trialed in human fertility clinics. Initial trials utilized sperm from both the woman’s partner and donor sperm in male infertility cases. While these initial procedures weren’t as precise as the current IUI experience today, they were considered a breakthrough for couples with infertility issues.
While Dr. Pincus’s work led to the first successful pregnancy through IUI, it wasn’t until the late 1970s and early 1980s that this method became available and accessible to the general public. With the advancing science of sperm preservation and sperm collection, it became increasingly feasible for fertility clinics to store sperm samples and utilize them in artificial insemination, marking significant advancements in fertility treatment that made IUI more accessible and allowing the procedure to be used clinically.
IUI also became more successful in the 1980s, with the advent of better sperm washing techniques for spermatozoa amplification. Sperm washing is the process of separating sperm from seminal fluid that may contain substances that inhibit fertilization or cause contractions of the uterus. Only the healthiest sperm are used, giving improved chances of success in IUI.
The first clinical use of IUI occurred in small, experimental settings during the 1960s, though it wasn't until the following decade that the procedure began to be utilized in clinical practice on a larger scale. The pivotal moment occurred when doctors began to understand the potential of IUI in treating male infertility, unexplained infertility, and cervical barriers that prevented sperm from reaching the egg. The technique also became an option for women who have normal ovarian function but whose cervical mucus is either hostile or inadequate to allow sperm to swim into the uterus.
In the 1980s, IUI was established as a formal medical procedure, and fertility clinics began to offer it as a standard treatment for various infertility-related issues. By now, IUI was being used more and more, not only to assist couples who had male infertility issues (including low sperm count or poor sperm motility) but also for women with ovulatory disorders, unexplained infertility, and cervical mucus problems.
IUI became very popular in the 1990s, as it turned out to be effective for many patients. By then, it was a staple of fertility treatments and was used to treat both male and female infertility problems. The treatment was less invasive and cheaper than IVF, so it became available to many couples. The success rates were much higher than traditional methods of insemination, and it was a potential answer for couples with no apparent reasons for infertility.
1990s – This was the decade when sperm preparation techniques also became more advanced, as sperm washing and the pre-treatment of sperm to enhance fertilization odds were developed. The introduction of ultrasound-guided IUI, which allows doctors to visualize where the sperm settles in the inner lining of the uterus, took the procedure’s accuracy and success rate to the next level.
IUI procedures began to integrate with treatments like ovulation induction as they developed and became more refined over time. The implementation of golden egg ideas in the form of ovulation induction stimulates the ovaries to generate more than one egg, increasing the likelihood of success. Today, IUI is often performed along with medications such as clomiphene citrate or gonadotropins to increase the success rate, especially in the case of women with ovulatory dysfunction.
Besides male infertility, IUI has also been used to address a variety of fertility issues, including women with endometriosis and unexplained infertility and even sperm donors. In the context of intrauterine insemination with controlled ovarian hyperstimulation (COH-IUI), the procedure has also become an integral part of the treatment of women who would otherwise not ovulate or would experience irregular ovarian activity due to other factors.
The first recorded uses of Intrauterine Insemination (IUI) in clinical practice predated the advent of ultrasound, and the technique, which relies only on menstrual flow to guide the timing of insemination, has seen significant advances in its application over the years. What started as an experimental method in the 1960s has developed into a mainstay of contemporary fertility therapies. For couples confronting male infertility or unexplained infertility, IUI is often a viable option due to its less invasive and more cost-effective approach compared to more complicated forms of ART like IVF. Despite the growing list of alternative treatments available, IUI still plays an important role in the world of fertility, showcasing the advancements in fertility treatment that have improved success rates for many couples.
