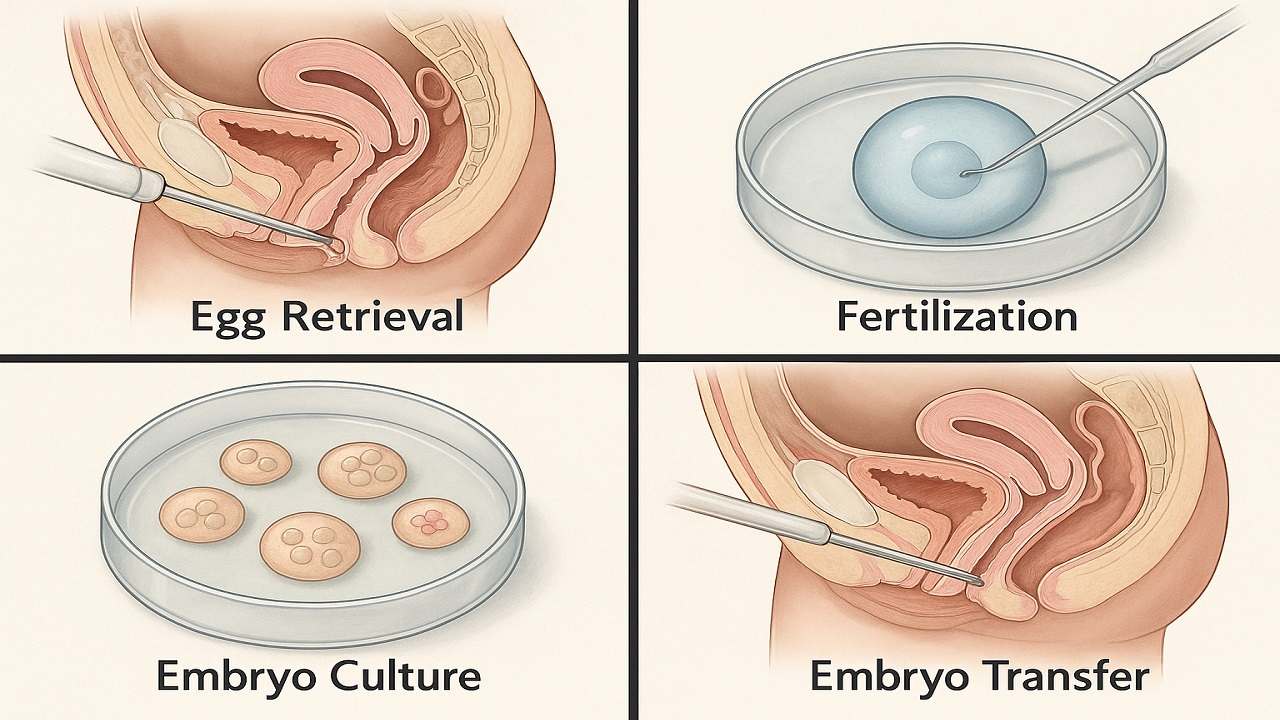
In Vitro Fertilization (IVF) process step by step, emphasising the importance of various stages such as ovarian stimulation, egg retrieval, fertilization, and embryo transfer in maximising the In Vitro Fertilization (IVF) Success Rate. It highlights how a thorough understanding of the procedure can prepare couples and individuals for their In Vitro Fertilization(IVF) journey, ultimately improving their chances of achieving a successful pregnancy.
The assisted reproductive technology (ART) least commonly used by the couple and single person facing infertility is in vitro fertilization (IVF). IVF involves fertilizing eggs outside the body and then implanting the resulting embryos into the uterus. While the IVF process might seem overly complicated and labor-intensive, breaking it up into its individual components helps future patients understand what to anticipate. This page will give you a comprehensive, step-by-step guide to the IVF process, from the first consultations to the last embryo transfer.
 STEP ONE: Ovarian Stimulation
STEP ONE: Ovarian Stimulation
- The IVF process begins with ovarian stimulation, or stimulation of the ovaries to produce a large number of eggs, or oocytes, as some may not grow properly or be viable, and the goal is to increase the number of mature eggs available for fertilization.
- Before commencing ovarian stimulation, women have a thorough assessment involving blood tests and ultrasounds to determine their ovarian reserve, hormone levels, and other general reproductive health.
- The patient begins daily gonadotropin injections, which are substances (such as FSH, follicle-stimulating hormone and LH, luteinizing hormone) that stimulate the ovaries to produce multiple eggs. Hormonal treatment, which typically starts on the second or third day of the menstrual cycle, lasts about ten to fourteen days.
- The patient will also be monitored for responses to the hormones and the development of eggs in the ovaries, frequenting the fertility clinic for regular ultrasounds and blood tests throughout the stimulation period.
 STEP TWO: Monitoring and Changing Medications
STEP TWO: Monitoring and Changing Medications
- With ovarian stimulation, the fertility team monitors the patient’s response to the drug closely with the help of blood testing and ultrasonic monitoring. The eggs should be developing properly, and the patient should avoid ovarian hyperstimulation syndrome (OHSS), a rare but potentially serious side effect.
- The size of the follicles fluid sacs containing the eggs as they mature is routinely measured by ultrasonic methods. There should be many follicles in each ovary.
- Blood tests measure hormone levels, especially estrogen, which should increase as the eggs develop.
- The fertility expert may adjust the medication dosages during this time if necessary to ensure the ovaries respond optimally and are not overstimulated.
STEP THREE: Transvaginal Aspiration - Egg Retrieval
- Next is egg retrieval, also known as aspiration, if the eggs are mature and the follicles are the right size. This is a very minor surgical procedure requiring anaesthsia.
- Method: The patient is given mild sedation or a local anesthetic for comfort. The egg retrieval procedure is performed under the guidance of ultrasound and requires that a thin, flexible needle be inserted through the vaginal wall and into the ovaries. The needle collects the matured eggs from the follicles.
- The egg retrieval procedure, which lasts anywhere between twenty and thirty minutes, Postoperatively, the patient receives short-term monitoring to ensure that any immediate complications have not arisen. Most women can return home the same day after a short period of rest.
- After egg retrieval, the patient’s eggs are sent to the lab, where they can be fertilized. The woman's body will also be closely monitored for signs of ovarian hyperstimulation syndrome (OHSS), a rare complication following egg retrieval.
STEP FOUR: Sperm Collecting and Preparation
- The male partner or sperm donor needs to provide a fresh sperm sample on the day of egg retrieval. These sperm are treated and primed for fertilization. This involves washing the sperm to remove non-motile sperm and debris and then isolating the healthier, more motile sperm.
- They examine the motility (movement), concentration, and shape, i.e., the morphology, of the sperm sample. Only the highest-quality sperm are selected for fertilization.
- If there are any issues with the quality of the sperm or in cases of male infertility, the fertility doctor might also use intracytoplasmic sperm injection (ICSI), where one single sperm is injected directly into an egg.
STEP FIVE: Fertilization
Once the eggs and sperm are mature, fertilization occurs in the lab. Eggs can be fertilized by two primary methods:
- Conventional IVF: The sperm and eggs are combined on a petri dish; fertilization happens naturally as the sperm penetrates the eggs themselves.
- If there are problems with male infertility or any other issues occur, a single sperm is directly injected into the egg to achieve fertilization. People often use this method when sperm quality is poor or when previous IVF attempts have failed.
- Once fertilization is complete, embryologists monitor the embryos for signs of development over the coming several days in order to establish the most viable embryos.
STEP SIX: Monitoring Embryo Culture
- The resulting embryos are then cultured for three to five days after fertilization. Embryologists monitor their progress during this time, reporting on aspects such as blastocyst development, the quality of embryos, and cell division. Grading is based on the appearance of the embryos, and the top-quality embryos are selected for transfer.
- Although many IVF clinics will transfer at Day 5 (the blastocyst stage), embryos are sometimes transferred on Day 3 (three days post-fertilization). This enables a more effective selection of the most viable embryos and increases the chances of successful implementation.
- Any viable embryo that isn't transferred can be frozen for use in future IVF cycles. This will be very useful for women who have multiple embryos.
STEP SEVEN: Embryo transfer
- The IVF process occurs during embryo transfer. It is a non-surgical procedure that generally does not need anaesthesia.
- The doctor will insert a thin, flexible tube through the cervix and into the uterus to deposit one or more healthy embryos. Typically quick and painless, the surgery may cause some women slight cramping.
- Transferring embryos is influenced by the age of the woman, the quality of the embryos, and any history of previous IVF processes. To reduce the risk of multiple pregnancies, only one or two embryos usually are implanted. Yet the fertility specialist may transfer more embryos given some conditions.
- Patients are usually sent home after resting for a while following the transfer of the embryos.
STEP EIGHT: Luteal Phase Support
- After the embryo transfer, the body needs additional support to ensure that the uterus is prepared to accept and sustain pregnancy in the embryos. Women are thus given luteal phase support, which may be delivered in progesterone via an oral pill, injectable, or vaginal suppository route. This treatment promotes early pregnancy and primes the uterine lining for implantation.
Step Nine: Test of Pregnancy
A blood test checks for pregnancy ten to fourteen days after the embryo transfer. Called a beta hCG test, this measures human chorionic gonadotropin (hCG), the hormone produced by a developing pregnancy.
- If the results show positive, that means implantation has occurred and the pregnancy is in progress. The patient will have ultrasounds and repeated blood tests to monitor the pregnancy.
- If the test is negative, the cycle was unsuccessful. The fertility specialist will discuss next steps, such as another IVF cycle, the use of frozen embryos, or alternative treatments.
- Return of pregnancy status at Day 30 (after 5–10 days of treatment period)
If the pregnancy test is positive, the patient will then be closely monitored with ultrasounds and blood tests to ensure the pregnancy is progressing. An ultrasonography scan will be conducted between six to seven weeks to confirm the fetal heartbeat and to assess whether it is a viable pregnancy.
Final Thought
IVF is a complex, multi-step process that requires attentive monitoring and collaboration between patient and fertility team. Everything from ovarian stimulation and egg harvesting to fertilization and embryo transfer is completely essential in maximising the chance of a pregnancy. While emotionally and physically challenging, with enough time and some patience, IVF has helped many couples and singles get their chance at the child they picture in their dreams. Having a good, rough-edged knowledge of the procedure will ensure that patients are better informed and prepared to embark on their IVF journey.