Laser-Assisted Hatching improves embryo implantation by gently opening the zona pellucida using advanced laser technology, supporting better IVF outcomes for select patients.



In the realm of assisted reproduction, Laser-Assisted Hatching has emerged as one of the most sophisticated laboratory techniques designed to boost embryo implantation potential. As in vitro fertilization (IVF) technology continues to evolve, embryologists now rely on micro-level precision tools to optimize every stage of the process. Among these, the laser-assisted approach plays a pivotal role in addressing one subtle yet crucial biological step, the embryo’s ability to “hatch” from its outer layer and implant successfully within the uterine lining.
This technology-driven procedure, performed under strict laboratory control, represents a blend of biological insight and advanced engineering. It exemplifies how fertility medicine continues to minimize barriers for patients who face complex infertility challenges.
Laser-Assisted Hatching is an advanced IVF laboratory technique that facilitates the embryo’s natural process of breaking out of its protective casing, the zona pellucida. In normal fertilization and embryo development, hatching occurs before implantation. However, in some cases, this natural step may be compromised due to the embryo’s structural or physiological conditions.
By using a highly precise laser to create a tiny, controlled opening in the zona pellucida, embryologists help the embryo “hatch” more easily, potentially increasing its ability to embed within the uterine wall. The laser system used emits focused bursts that are powerful enough to alter the outer shell without transmitting heat or damaging the delicate cells within.
This delicate balance between technology and biology underpins the safety and effectiveness of the procedure.
Embryo hatching is a prerequisite for successful implantation. The outer shell, while offering protection during early development, can in some situations become a barrier rather than a safeguard. Laser-Assisted Hatching seeks to overcome that limitation by giving the embryo mechanical support to complete the hatching phase.
The principal goal of the procedure is not to force hatching but to facilitate a natural biological milestone through technological support. This precise, laser-based intervention helps balance two key aspects: maintaining embryo integrity while increasing its implantation competence.
At its core, Laser-Assisted Hatching aims to:
By enhancing this crucial step, fertility specialists can significantly refine the conditions for pregnancy success.
While the technique can theoretically be applied to any embryo, specialists recommend Laser-Assisted Hatching for selected patient groups where there is a higher likelihood of implantation difficulty. These cases are identified through clinical assessment and detailed reproductive history.
This selective approach ensures that the technique is used judiciously, maximizing benefits while minimizing unnecessary interventions.
The Laser-Assisted Hatching process takes place in a sterile laboratory environment immediately before embryo transfer. The embryo, typically at the blastocyst or cleavage stage, is stabilized under a high-magnification microscope connected to a precision laser instrument.
The procedure usually takes only seconds per embryo and is performed by highly trained embryologists using advanced laser systems that guarantee reproducibility and precision.
Though generally regarded as safe and minimally invasive, Laser-Assisted Hatching is classified as an IVF add-on a supplementary technique rather than a core step. Its success largely depends on clinical indication and lab expertise rather than universal application.
Patients should always discuss the clinical rationale, potential benefits, and costs before opting for this IVF enhancement. Transparency in counseling builds trust and ensures well-informed decisions.
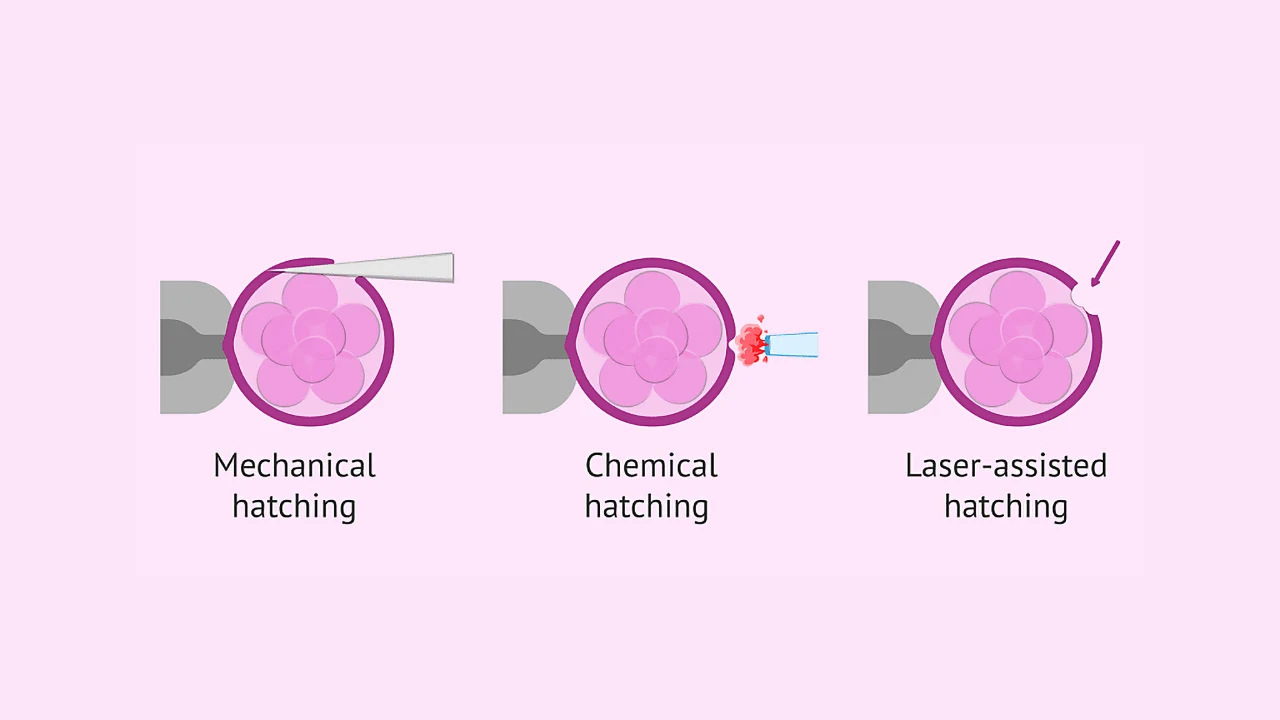
Before laser technology became the gold standard, embryologists used mechanical or chemical methods such as acid Tyrode’s solution to weaken or thin the zona pellucida. These earlier approaches carried higher risks of embryo injury and lacked the fine control that lasers now provide.
This comparison highlights why Laser-Assisted Hatching is now favored in modern IVF laboratories for its precision, safety, and reproducibility.
The integration of Laser-Assisted Hatching into fertility programs underscores an ongoing ethical conversation within reproductive medicine. As with all IVF add-ons, specialists are urged to evaluate cost–benefit dynamics and patient-specific indications.
Ethical practice demands that the technique be positioned not as a guaranteed success enhancer, but as a scientifically justified tool for certain challenging cases. Responsible fertility centers emphasize informed consent and transparency regarding expected outcomes, aligning with current reproductive ethics frameworks that prioritize patient autonomy and medical prudence.
Advancements in reproductive biotechnology continue to refine how embryologists support early developmental stages. Future iterations of Laser-Assisted Hatching will likely integrate artificial intelligence and computer vision to determine optimal laser intensity, position, and energy exposure for each embryo.
Emerging studies also explore combining assisted hatching with time-lapse imaging and embryo genomics for ultra-personalized embryo selection. As fertility clinics move toward more data-driven approaches, techniques like laser-assisted hatching will become not just interventions but elements of predictive reproductive modeling, enhancing precision, safety, and success predictability.
In conclusion, Laser-Assisted Hatching represents a marriage between modern technology and biological insight, enhancing one of the most critical steps in embryonic development the moment of implantation. Though classified as an IVF add-on, it holds remarkable promise for specific patient groups where natural hatching presents a barrier.
By enabling a clearer path for the embryo to implant, this technique transforms a potential obstacle into an opportunity for success. Its precision, safety, and scientific rationale make it an exemplary model of how innovation continues to redefine modern fertility care one microscopic laser pulse at a time.
