Sperm quality to improve after quitting smoking or alcohol, representing crucial knowledge that can significantly influence family planning strategies. Recent clinical evidence demonstrates that sperm parameters undergo remarkable recovery following cessation of these substances, with improvements beginning within weeks and reaching optimal levels within three to six months.



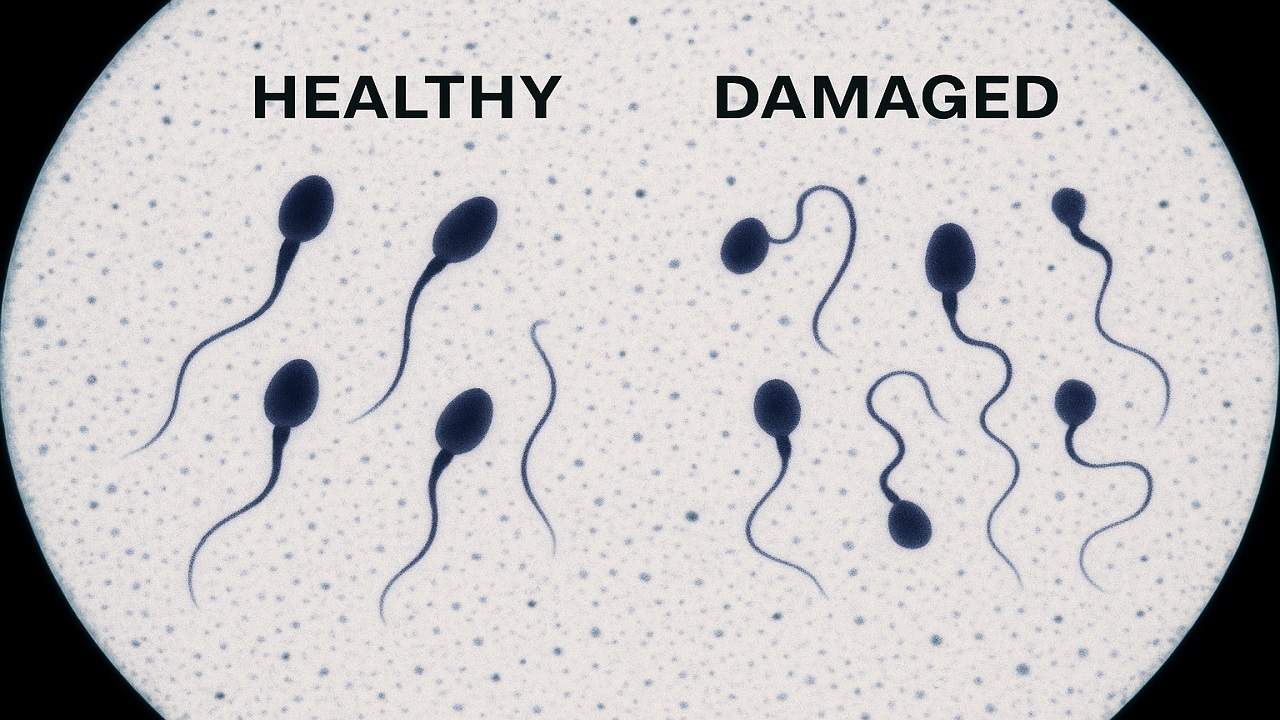
The biological foundation underlying fertility recovery lies in the intricate process of spermatogenesis, the 74-day cycle through which mature sperm cells develop from primitive germ cells. This knowledge provides both hope and a scientific framework for understanding why patience is essential in the fertility restoration process, as the body requires time to produce an entirely new generation of healthy sperm cells free from the toxic effects of smoking and alcohol.
Understanding how long it takes for sperm quality to improve after quitting smoking or alcohol begins with comprehending the sophisticated biological process of sperm development. Spermatogenesis occurs within the seminiferous tubules of the testes and involves three distinct phases that collectively span approximately 74 days. This timeline represents the entire journey from primitive germ cells to fully mature spermatozoa capable of fertilization.
The recovery process is fundamentally tied to this 74-day cycle, which includes:
This biological timeline explains why significant improvements in sperm quality typically become apparent after approximately three months of substance cessation. The sperm present in ejaculate at the time of quitting were exposed to toxins during their development, while those produced three months later represent the first generation of completely toxin-free sperm cells.
Clinical research provides compelling evidence regarding how long it takes for sperm quality to improve after quitting smoking or alcohol, with smoking cessation studies showing particularly robust data. A landmark investigation involving 48 men who successfully quit smoking after consuming at least 20 cigarettes daily for over one year revealed significant improvements within just three months.
The specific improvements observed at three months post-cessation included:
Extended studies tracking participants for six months demonstrated even more dramatic improvements, with progressive motility increasing by 104% (from 20.7% to 42.28%) and abnormal morphology decreasing from 69.32% to 40.82%. These findings underscore that while initial improvements occur at three months, continued abstinence yields progressively better results.
Research examining how long it takes for sperm quality to improve after quitting smoking or alcohol reveals that alcohol cessation may produce even more rapid results than smoking cessation. A remarkable case study documented a man who progressed from complete azoospermia (absence of sperm) to normal semen parameters within just three months of alcohol withdrawal.
The recovery timeline for alcohol cessation demonstrates:
This accelerated recovery pattern appears related to alcohol's primary impact on hormonal regulation rather than direct cellular damage. When alcohol consumption ceases, the hypothalamic-pituitary-gonadal axis can rapidly restore normal testosterone production and spermatogenesis regulation. Studies indicate that chronic alcohol consumption particularly affects the hormonal environment necessary for sperm production, but this damage proves largely reversible upon cessation.
Understanding how long it takes for sperm quality to improve after quitting smoking or alcohol requires examining how different sperm parameters respond to cessation. Research reveals that various aspects of sperm quality recover at different rates, providing insight into the complex nature of fertility restoration.
Sperm concentration and count typically show the earliest and most dramatic improvements:
Sperm motility demonstrates progressive improvement over time:
Sperm morphology proves most resistant to improvement:
This differential recovery pattern suggests that men seeking to optimise fertility should maintain cessation for at least six months to achieve a comprehensive sperm quality improvement.
Several variables affect how long it takes for sperm quality to improve after quitting smoking or alcohol, making individual recovery timelines somewhat unpredictable. Understanding these factors helps set realistic expectations and optimise cessation strategies.
Duration and intensity of substance use significantly impact recovery speed:
Age at cessation influences the restoration process:
Overall health status affects the body's ability to restore normal sperm production:
An often-overlooked aspect of how long it takes for sperm quality to improve after quitting smoking or alcohol involves the restoration of genetic integrity within sperm cells. Both smoking and alcohol consumption significantly increase sperm DNA fragmentation, potentially affecting fertilization success and offspring health.
Research on DNA fragmentation recovery reveals:
Studies demonstrate that sperm DNA fragmentation can improve dramatically with shortened abstinence periods, suggesting that the epididymal storage environment plays a crucial role in maintaining genetic integrity. Men with elevated DNA fragmentation often benefit from more frequent ejaculation during the recovery period to minimise exposure to oxidative damage.
While understanding how long it takes for sperm quality to improve after quitting smoking or alcohol provides valuable timeline expectations, implementing supportive strategies can potentially accelerate and enhance the recovery process.
Nutritional optimisation supports cellular repair and regeneration:
Lifestyle modifications complement cessation efforts:
Medical monitoring ensures optimal recovery:
The question of how long it takes for sperm quality to improve after quitting smoking or alcohol extends beyond immediate parameter improvements to encompass long-term fertility outcomes and family planning considerations. Research indicates that men who successfully maintain cessation experience sustained fertility benefits that can significantly impact conception success rates.
Assisted reproductive technology outcomes improve markedly following cessation:
Natural conception probability increases substantially:
The evidence demonstrates that the investment in cessation yields long-term fertility dividends that extend well beyond the initial recovery period. Men who maintain abstinence from smoking and alcohol create optimal conditions not only for conception but also for healthy pregnancy outcomes and offspring development.
Understanding how long it takes for sperm quality to improve after quitting smoking or alcohol empowers men to make informed decisions about their reproductive health and family planning strategies. The scientific evidence consistently demonstrates that significant improvements occur within three to six months, with the potential for continued enhancement over longer periods.
While the 74-day spermatogenesis cycle provides the biological framework for recovery, individual factors influence the timeline and extent of improvement. The decision to quit smoking or alcohol represents one of the most impactful steps men can take to optimise their fertility potential and contribute to successful conception and healthy offspring development.
