Fertility preservation options before chemotherapy or radiation in both male and female. Fortunately, fertility preservation techniques allow individuals to safeguard their ability to have biological children before undergoing treatment. These methods provide hope for future parenthood, even after aggressive cancer treatments.
Options for Fertility Preservation Before Chemotherapy or Radiation
Chemotherapy and radiation are potent tools in the cancer treatment arsenal, effectively treating a variety of cancer types. But such treatments can sometimes affect fertility, particularly when they affect the reproductive organs or reproductive cells. The good news is that thanks to advances in medical science, it is possible to preserve fertility prior to the initiation of cancer treatment. By doing so, individuals can access a variety of procedures that may enable them to have biological children in the future, even after undergoing potentially fertility-diminishing treatments. By learning about all the fertility preservation options out there, those going through cancer treatment can be in a position to make informed decisions for their futures.
Why Fertility Preservation Matters
Chemotherapy kills rapidly dividing cells and therefore may cause fertility issues because they compromise reproductive cells (such as eggs in women and sperm in men). And in fact, the degree of fertility loss that accompanies cancer treatment varies due to a number of factors, including the kind of cancer, the particular treatment given, the age of the individual, and the state of their reproductive organs before treatment began.
If a woman undergoes fertility preservation by freezing her eggs or embryos before treatment, her ability to conceive a family at a later date is preserved. It's important to understand that fertility preservation is a hopeful step that puts individuals in control of their reproductive health.
1. Women’s Fertility Preservation Options
Oocyte Cryopreservation (Egg Freezing)
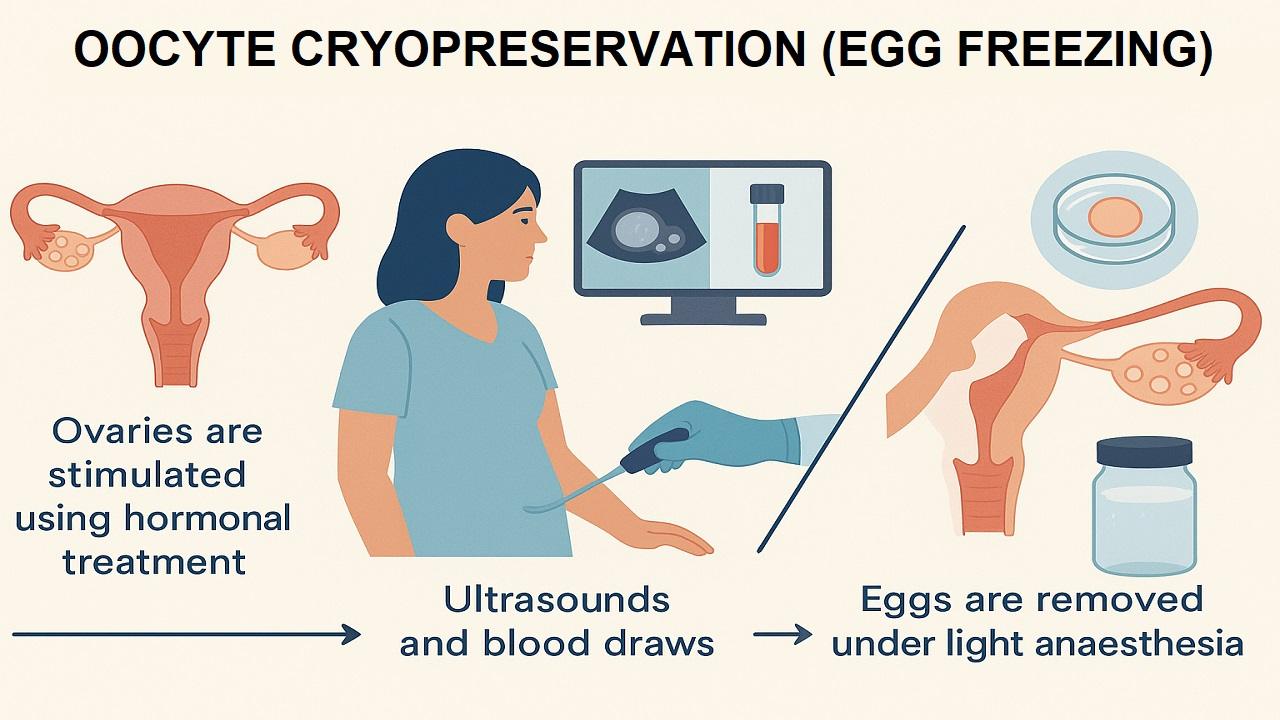
- One of the most recommended methods of fertility preservation for women is egg freezing. This process involves hormones that stimulate the ovaries to produce multiple eggs, which are then harvested and frozen for future use. Egg freezing gives women viable eggs for the future, even a future when cancer treatment has damaged their fertility.
- Process: Ovaries are stimulated using hormonal treatment, which takes around 10–14 days. In the meantime, the woman is serially monitored with ultrasounds and blood draws. When the eggs are ready, they are removed under light anesthesia.
- Best Candidates: If you are single or not ready to use sperm when the eggs are frozen. It works best for women age 35 and under (egg quality tends to decrease with age).
Embryo Freezing
- Embryo freezing is a great option for women in a relationship or those who are prepared to use sperm for fertilization. This approach fertilizes the eggs with sperm before subsequently freezing the embryos that are created. Embryo freezing is often favored over egg freezing because embryos are more resistant to the freezing process and typically have a greater success rate after thawing.
- Procedure: Like egg freezing, eggs are harvested through hormonal stimulation. Next, they add sperm, either from a partner or a donor, to fertilize the eggs. The embryos are cultured for a few days before being frozen.
- Control Factor: This option works best for women in committed relationships with access to sperm (from a partner or a donor). It is also generally much more successful than egg freezing, particularly for women over 35.
Ovarian Tissue Freezing
- Ovarian tissue freezing is one option for women who require immediate treatment for cancer and wish to not delay that treatment for the time required for ovarian stimulation (such as in young girls or women with aggressive cancers). This involves extracting and freezing a small amount of ovarian tissue that contains immature eggs.
- Procedure: A portion of ovarian tissue is surgically removed and frozen. The tissue can then be transplanted back into the woman’s body after treatment to restore ovarian function.
- Who is a Suitable Candidate: This approach is typically suggested for women who can't afford the time to freeze eggs or embryos given their cancer's TSA (time-sensitive action) plan. It is also possible for prepubescent girls who have yet to start their periods.
Hormonal Therapy: Ovarian Suppression (With GnRH Agonists)
- Other women opt for mass ovarian suppression as a way to guard their ovaries from the ravages of chemotherapy. This strategy involves the use of hormones known as GnRH agonists to temporarily "shut down" the ovaries, reducing the risk of chemotherapy damaging them during E & O therapy.
- Process: GnRH agonists are generally given as an injection before and during chemotherapy. The goal of such a protocol aims to suppress the ovarian functionality, therefore reducing exposure to the chemotherapy utilizing it.
- Best Candidate: This approach may work for women who cannot afford to put off treatment in order to retrieve eggs or freeze embryos. But it is not as effective as freezing eggs or embryos and is often treated as a supplemental option.
2. Male Fertility Preservation Options-Oligozoospermia and Infertility Treatment
Sperm Storage (Freezing of Sperm)

- Sperm banking is the most established fertility preservation method for men. Sperm banking, in which sperm is collected and frozen prior to the beginning of cancer treatment, enables men to keep their options for having biological children open long-term.
- Process: Fellas are usually requested to submit a sperm sample via masturbation. Then the sperm is processed, analysed, and frozen for future use. Men can potentially bank multiple samples to increase their success odds later.
- Best Candidates: This approach works well for men of any age who have enough time to prevent cancer with this approach before starting prostate cancer treatment. It is a quick and easy process with non-invasive procedures and has been found to get very good results for men who want to preserve their fertility.
Testicular Tissue Freezing
- For prepubescent boys who cannot yet produce sperm, or for men who cannot give a sperm sample at the time of cancer treatment, freezing testicular tissue, which contains immature sperm that may later mature in a lab if needed, may be an option. In this procedure, a small piece of testicular tissue is removed and frozen. The tissue can then be used to extract sperm, which can be used in assisted reproduction.
- Process: A small piece of testicular tissue is needed; thus, a minor surgical procedure would be needed. The tissue is subsequently frozen and stored.
- Best For: This is often the choice for prepubescent boys or men who are unable to provide a sperm sample. It may also be an option for men who are undergoing treatments that could harm sperm production.
The Future of Fertility Preservation
Now, these innovative fertility preservation techniques provide cancer survivors with more opportunities than ever to preserve their reproductive health prior to chemotherapy, radiation, or surgery. The field of these technologies is progressing further there is even higher hope for parenthood in the future as technology and science are improving the results and outcomes of these techniques. Many people who have stored their gametes before cancer treatment end up starting families via assisted reproductive technologies, such as IVF.
In addition, scientists are always looking at new ways to advance fertility preservation techniques, from ovarian tissue re-implantation to potentially growing eggs or sperm back from frozen tissue someday.
Conclusion
Fertility preservation is a way for cancer treatment patients to preserve their ability to conceive biological children in the future. There are also options like egg freezing, embryo freezing, sperm banking, and ovarian tissue freezing. And that when we act early and speak with a medical professional about fertility preservation, we can take charge of our reproductive health and allow for peace of mind that we are preserving our fertility for a future. These alternatives give many hope that they can pursue their dreams of parenthood even after undergoing cancer treatment.